The Science of Breast Augmentation: Implants, Anatomy, and Outcomes
Estimated reading time: 4 minutes
Table of contents
The Evolution of the Procedure
Breast augmentation is primarily performed through the surgical placement of an implant or, less commonly, through autologous fat transfer. While the FDA placed a restriction on silicone-filled implants in 1992 due to perceived risks, extensive research failed to link silicone to systemic disease. In 2006, the ban was lifted, and by 2017, the majority of patients chose cohesive gel silicone implants—often referred to as "gummy bear" implants—for their natural feel and lower rupture rates.
Surgical Anatomy: The Surgeon's Map
The female breast is a complex structure located on the anterior chest wall. Successful augmentation requires a deep understanding of its boundaries and vascularity:
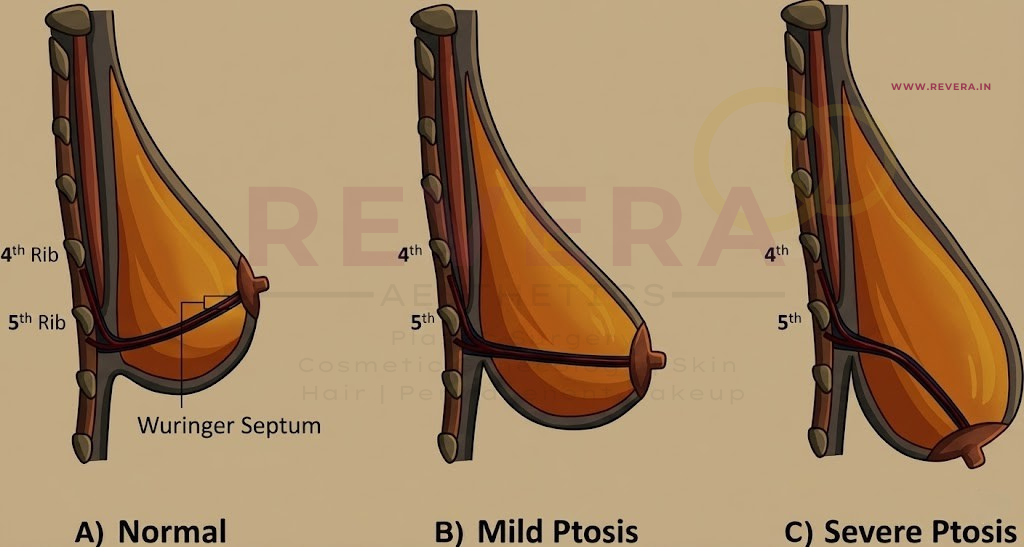
- The Boundaries: Inferiorly, the breast is defined by the inframammary fold (IMF), a dermal structure formed by the fusion of the superficial and mammary fascia. Medially lies the sternum, and laterally, the edge of the latissimus dorsi.
- The Posterior Wall: The pectoralis major and minor muscles form the posterior boundary of the breast.
- Blood & Nerve Supply: Primary vascularization comes from the internal and external mammary arteries and intercostal perforators. Sensation is primarily governed by the third through fifth intercostal nerves.
Technical Choices: Implants and Placement
Surgeons must choose between two primary filler materials and two placement pockets, each with distinct clinical profiles.
1. Implant Types
- Saline-Filled: These have a silicone outer shell and are filled with sterile saline during surgery. They offer volume variability (usually a 25 to 50 mL range) but are more prone to "rippling" in thin patients.
- Silicone-Filled: These utilize a viscous, cohesive silicone gel. They are preferred for patients with minimal soft tissue because they provide a softer, more natural feel.
2. Pocket Placement
- Subglandular (Above the muscle): Offers an easier recovery but may have a higher incidence of capsular contracture when using textured implants.
- Submuscular (Beneath the pectoralis muscle): Provides better coverage of the implant edges and may lower contracture rates, though recovery can be more intense.
3. Incision Locations
Common access points include the inframammary crease (most common), transaxillary (armpit), and periareolar (around the nipple).
Complications and Safety Monitoring
While augmentation is considered safe with high satisfaction rates (70–80%), it is not a "lifetime" procedure. Implants typically have an estimated lifespan of 15 to 20 years.
| Complication | Description |
| Capsular Contracture | A tightening of the tissue capsule around the implant, graded on a scale of 1 to 4. Often linked to sub-clinical biofilm formation. |
| ALCL Risk | A rare possibility of Anaplastic Large Cell Lymphoma (ALCL) has been reported, potentially linked to specific types of textured implants. |
| Silent Rupture | Silicone leaks can be asymptomatic. The FDA recommends MRI screening every 2 years to detect subclinical leaks. |
| Hematoma/Seroma | Early postoperative fluid collections that may require drainage. |
Interprofessional Coordination for Better Outcomes
The study emphasizes that optimal outcomes rely on an interprofessional team:
- Nurses: Crucial for providing informed consent and ensuring patients understand the need to discontinue smoking to prevent wound complications.
- Pharmacists: Play a role in managing postoperative pain and ensuring antibiotics are used correctly to prevent the "biofilm" that can lead to capsular contracture.
- Surgeons: Must manage patient expectations and identify psychological instability or Body Dysmorphic Disorder before proceeding.
Frequently Asked Questions (FAQ)
Q: At what age can someone get breast implants? A: Saline implants are FDA-approved for augmentation in patients 18 and older. Silicone implants are approved for patients 22 and older, though they are often used "off-label" for younger patients when indicated.
Q: Do I really need an MRI every 2 years? A: Yes, the FDA recommends this for silicone implants because a "silent rupture" cannot be felt or seen during a physical exam.
Q: Does texturing prevent the implant from moving? A: Yes, texturing is specifically used in shaped (form-stable) implants to prevent them from rotating, which would distort the breast shape.
Reference
Social Media Hashtags
#BreastAugmentation #PlasticSurgery #MedicalEducation #Implants #SalineVsSilicone #PatientSafety #StatPearls #GummyBearImplants #SurgicalAnatomy #WomensHealth