Lollipop vs. Anchor: Which Breast Reduction Technique is Safer?
The Scar Debate: Less is More?
When you consider breast reduction surgery, scarring is often a top concern. Traditionally, surgeons used the Wise-Pattern (or “Anchor”) technique. This leaves a scar around the areola, down the middle, and along the crease underneath the breast.
However, a newer technique called the Vertical Scar (or “Lollipop”) reduction has gained popularity. It eliminates the horizontal scar underneath the breast, leaving only a vertical line.
Patients often ask: Is the “Lollipop” technique just as safe? Can it handle large reductions? A study from the University of Illinois answers these questions.
The Study: Comparing 200 Breasts
Researchers wanted to compare these two popular methods directly. They conducted a “matched cohort study,” meaning they paired patients with similar ages and breast sizes to get a fair comparison.
- Group A: 100 breasts operated on using the Superomedial Pedicle Vertical technique (“Lollipop”).
- Group B: 100 breasts operated on using the Traditional Inferior Pedicle Wise-Pattern technique (“Anchor”).
This was a significant study because it looked at outcomes over a 3-year period.
The Results: Equal Safety, Less Scarring
The findings were reassuring for anyone hoping for fewer scars.
- Large Reductions: The Vertical technique successfully handled large reductions. The average tissue removed was 815g (Vertical) versus 840g (Anchor) per breast.
- Complications: There was no statistical difference in complications between the two groups. Healing issues and safety profiles were essentially the same.
- Symptom Relief: 100% of patients in both groups achieved relief from their symptoms (like back and neck pain).
The Verdict: The Vertical “Lollipop” reduction is a safe and effective alternative to the traditional “Anchor” method, even for larger breasts.
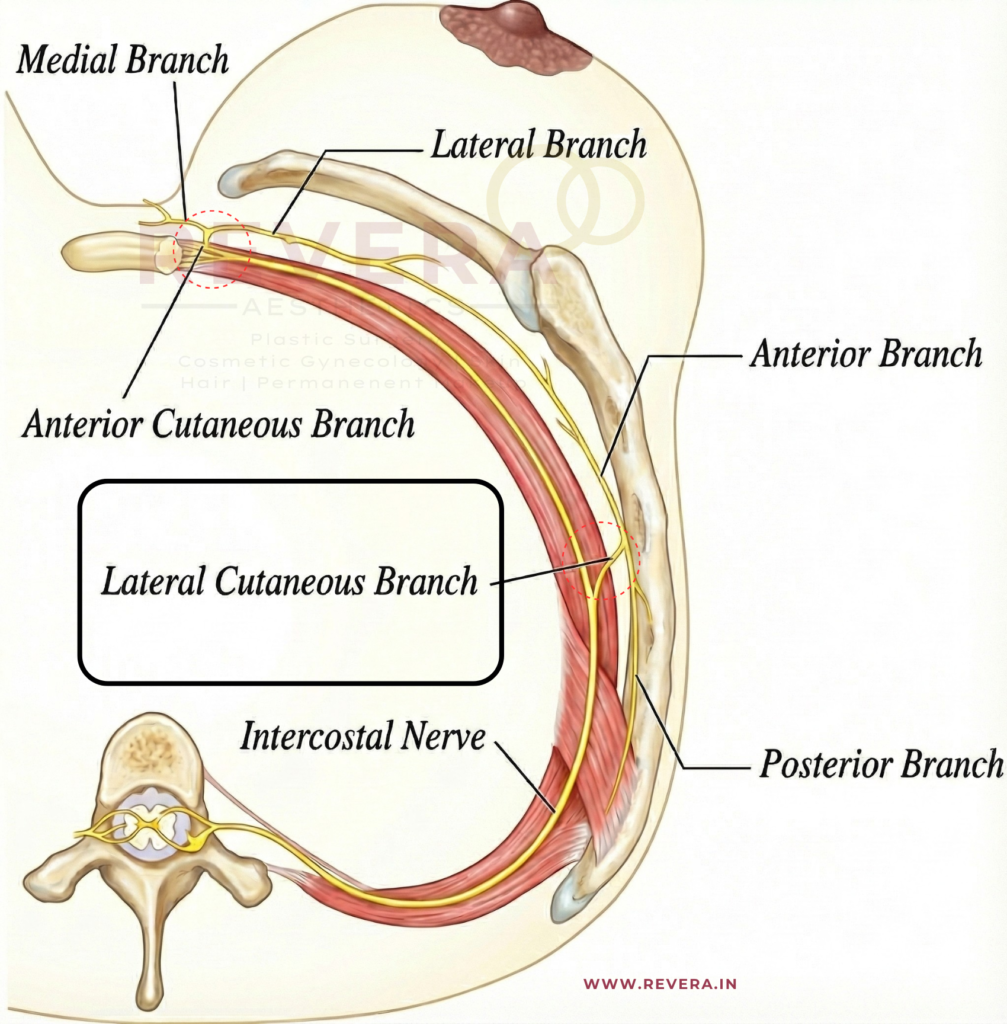
A Deeper Dive: It’s All About Blood Supply
In the accompanying discussion, expert surgeon Dr. Elizabeth Hall-Findlay highlights why the “Vertical” technique works so well. It often comes down to the “pedicle”—the bridge of tissue that carries blood to the nipple.
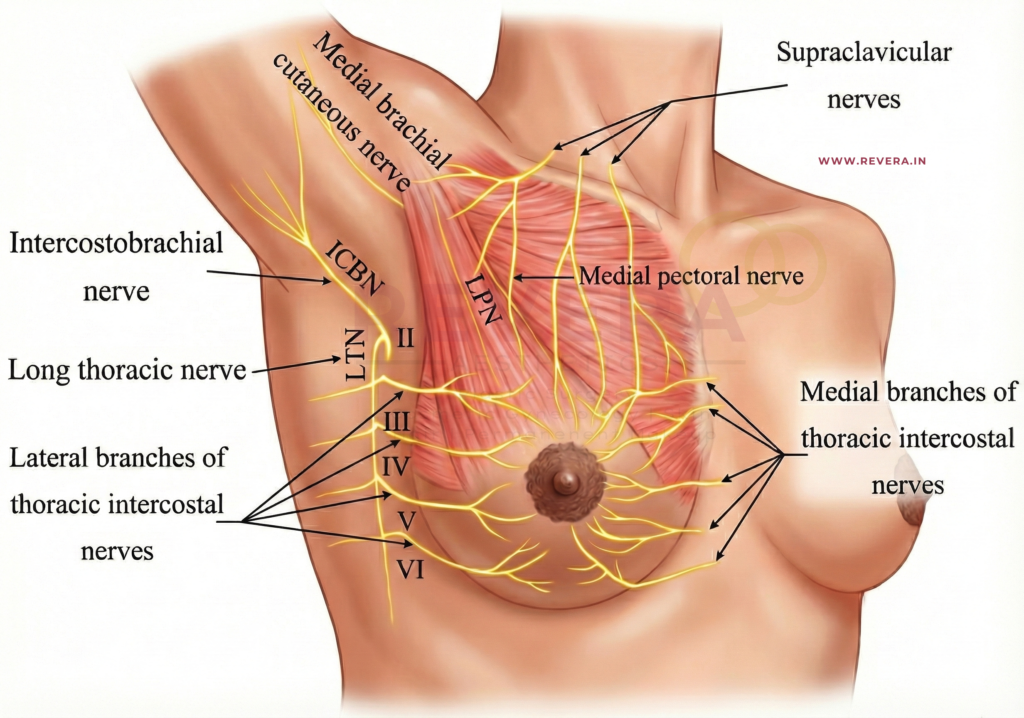
Dr. Hall-Findlay explains that the breast has four major arteries supplying it.
- Inferior Pedicle (Traditional): Relies on the deep artery from the 4th interspace.
- Medial/Superomedial Pedicle (Vertical): Relies on strong arteries from the 2nd or 3rd interspace.
She notes that a true Superomedial Pedicle is particularly robust. It incorporates the “very strong descending artery” from the second rib space. This provides a powerful “dual” blood supply, making it a reliable choice for keeping the nipple healthy during surgery.
Which Is Right for You?
This study proves that you do not necessarily need an “Anchor” scar just because you require a large reduction. The “Lollipop” technique offers excellent functional and aesthetic outcomes with a shorter scar.
However, anatomy varies. Your surgeon will choose the “pedicle” and scar pattern that best fits your specific blood supply and body shape.
References
- [1] Antony, Anuja K. M.D., M.P.H.; et al. “A Matched Cohort Study of Superomedial Pedicle Vertical Scar Breast Reduction (100 Breasts) and Traditional Inferior Pedicle Wise-Pattern Reduction (100 Breasts): An Outcomes Study over 3 Years.” Plastic and Reconstructive Surgery 132(5):p 1068-1076, November 2013.
- [2] Hall-Findlay, Elizabeth J. M.D. “Discussion: A Matched Cohort Study of Superomedial Pedicle Vertical Scar Breast Reduction… An Outcomes Study over 3 Years.” Plastic and Reconstructive Surgery 132(5):p 1077-1078, November 2013.