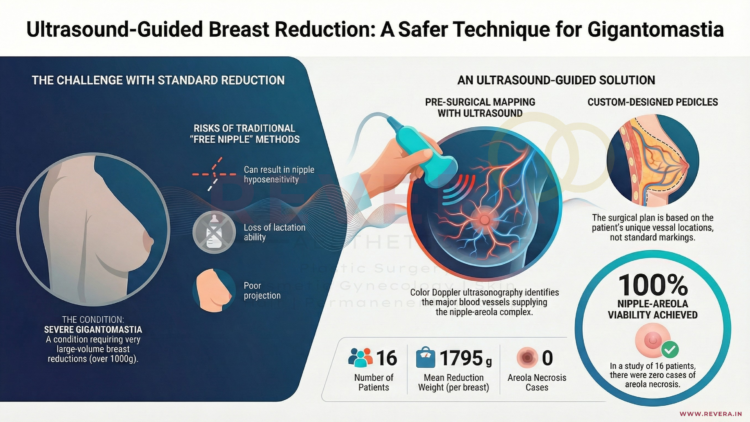
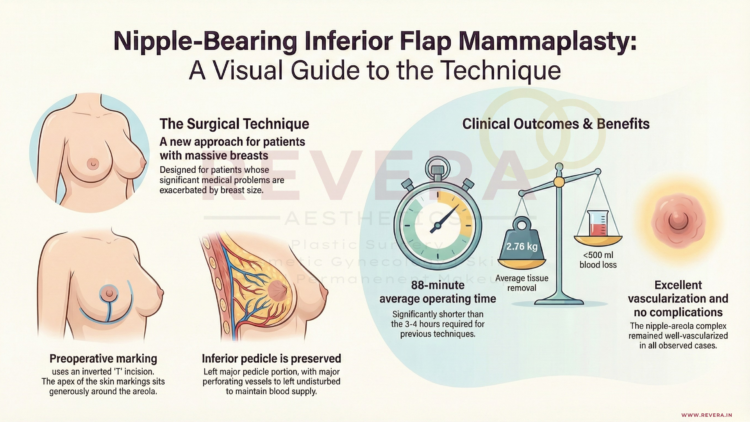
The Vertical “Lollipop” Scar: Now for Large Breasts – Breast Reduction
Can Large Breasts Have Smaller Scars?
In the past, patients with very large breasts (resection weights over 700g) were almost always given an “Anchor” scar. Surgeons believed the Vertical (or “Lollipop“) technique only worked for small reductions. They feared that the vertical scar would not be strong enough to hold the weight of a larger breast over time.
However, a massive study published in Plastic and Reconstructive Surgery has changed that thinking.
Researchers analyzed 500 breast reductions in 250 overweight patients. The research was conducted in Ulm, Germany, and Padova, Italy. They used a modified version of the “Lejour Technique” to prove that large breasts can achieve excellent results with fewer scars.
The Modifications: Making the Vertical Technique Stronger
The standard vertical technique can be difficult for large breasts. Therefore, the authors introduced several key modifications to make it more reliable.
1. Central Undermining (No Liposuction)
Instead of using liposuction to reduce volume, the surgeons used a “step-wise” surgical approach. They moved the tissue centrally and atraumatically. This preserves the best possible blood supply to the skin and nipple.
2. The “Three H Points” Fixation
This is the most critical part of the modification. A common problem with vertical reductions is “bottoming out.” This happens when the breast tissue sinks over time, making the bottom of the breast look too heavy.
To prevent this, the surgeons fixed the submammary fold (the crease under the breast) using three H points. These points act as a “pivot.” They anchor the internal tissue so it cannot sag later.
3. Adjusted Pleated Sutures
The vertical scar is often “pleated” or gathered during surgery. The authors adjusted this technique to match the specific retraction ability of the patient’s skin. For very large reductions, they occasionally combined it with a small horizontal line to ensure a smooth finish.
The Results: 94% Success Rate
The study tracked 250 patients for an average of 4.2 years. This long-term follow-up is important to see if the shape holds up.
- Large Reductions: The average tissue removed was nearly 1,000g per breast (over 2 lbs).
- Patient Outcomes: 94% of patients rated their results as “Very Good” or “Good”.
- Safety: The complication rate was 14%, which is comparable to traditional techniques.
Conclusion: A New Standard for Large Breasts
This research proves that the vertical technique is no longer just for “small” cases. It is a highly effective standard technique for larger breasts.
By using the “Three H Points,” surgeons can simplify the technique while reducing the visible scarring. If you have been told you are “too large” for a vertical reduction, this study shows that a modified approach can offer the smaller scar you want with the stability you need.
——————————-
Ask yourself “Who is the Best Plastic Surgeon Near Me?”.
Contact us to know if you are a suitable candidate for Breast Reduction.
Revera Clinic caters with the Best Plastic Surgeon in Hyderabad!
Frequently Asked Questions (FAQ)
Q: Does this technique work if I am overweight?
A: Yes. This study specifically looked at overweight patients with an average resection weight of over 900g per breast.
Q: Will the “pleated” scar look bumpy?
A: Initially, the vertical scar may look gathered. However, the study adjusted the sutures to the skin’s natural ability to retract. Over time, these lines typically flatten and fade significantly.
Q: What is the main benefit over the “Anchor” scar?
A: The primary benefit is the reduction of aesthetic deficiencies. You avoid the long horizontal scar across the chest, resulting in a more natural look in clothing and swimwear.
Reference
Hofmann, Albert K. M.D.; et al. “Breast Reduction: Modified ‘Lejour Technique’ in 500 Large Breasts.” Plastic and Reconstructive Surgery 120(5):p 1095-1104, October 2007.